Inside the ‘Covid Triangle’: a catastrophe years in the making | Free to read

Roula Khalaf, Editor of the FT, selects her favourite stories in this weekly newsletter.
Manish Shah knew it was only a matter of time before he was struck by coronavirus.
When the pandemic first hit the UK, the pharmacy where he works in Dagenham, east London, put in strict protocols on mask-wearing and physical distancing. But as the more aggressive variant of the virus raged through this part of the capital over the winter, more and more sick people turned to Shah for help.
“A lot of minicab and Uber drivers came to see me. They showed classic symptoms of the virus, but they kept saying things like: ‘Just give me something for the sore throat, cough syrup or something,’” he says. “I told them time and again to get a Covid test, but they just did not want to get a test or go to the doctor because they knew they could not afford to isolate.”
The pharmacy’s NHS contract meant that staff had to provide clinical services in partnership with local primary care networks. “We could not refuse anyone, even those not wearing a mask,” says Shah. “This is how I got the virus.”
Then he took it home. As with many south Asian families Shah, 56, lives in a multigenerational household. “When I started showing symptoms, I straightaway booked an apartment through Airbnb to isolate from my elderly parents.” But soon his father, who has Alzheimer’s, also fell sick, struggling to breathe. “To save my mum, both of us moved to the rented flat. My sister then had to come and help look after mum as she has Parkinson’s. Three days later, mum started showing symptoms. Then so did my sister.”
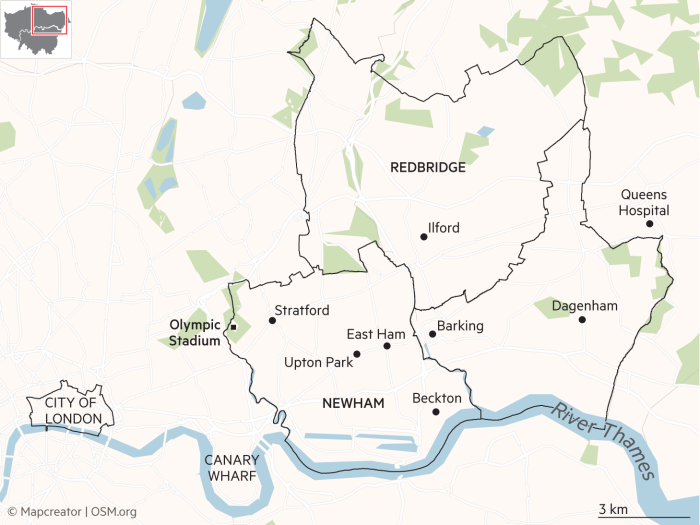
While coronavirus has inflicted extraordinary suffering across the country, the corner of east London in which Shah lives and works has been so pummelled that it has become known as the “Covid Triangle”. At one point during the peak of the second wave, the three boroughs that made up this triangle — Barking and Dagenham, Redbridge and Newham — were competing for the highest rate of infections in the whole country. In Barking and Dagenham, one in 16 people was reported to be infected.

Within this area, a high proportion of the workforce are either essential staff who cannot stay at home — like Shah — or those forced out to work by job insecurity. “Others that worked in takeaway restaurants told me: ‘I have to go into work, otherwise they will find someone else and I won’t have a job,’” he says. “These people had to keep going because of their financial circumstances.”
As the more contagious mutation sent death rates skyrocketing locally, it also exposed a complex web of deeper problems that have built up over many years. In particular, the increased exposure to the virus collided with the problems faced by an already susceptible population, many of whom suffered from comorbidities and poorer health outcomes.
High levels of deprivation and job insecurity, vast income inequality, housing discrimination and medical disparities have long had a severe impact on the tangle of communities and ethnic minority populations that live in these boroughs. But when combined with the necessity to go to work, to take public transport and to share space in densely packed housing, they also provided the perfect breeding ground for a deadly virus. The domino effect would prove catastrophic.
The odds were stacked against this part of London long before the arrival of coronavirus. For some, the ticking time bomb of economic deprivation and public health disparities was evident from the start. “This is a community scarred with inequality,” says Rokhsana Fiaz, the mayor of Newham. “Given that landscape and context, we knew it was going to hit us hard — we just didn’t know how hard.”
Between March and April 2020, during the first wave, Newham had the highest age-standardised mortality rate in England and Wales, at 144.3 deaths per 100,000, compared with 25 in some wealthier areas. While saving lives was the all-consuming priority, Fiaz knew the economic impact was also going to be significant.

Comprised of 350,000 residents and more than 200 languages and dialects, Newham was the pocket of east London showcased to the world when the UK hosted the 2012 Olympics. This was meant to mark a turning point for one of the country’s poorest areas.
Yet despite £9bn in spending and its proximity to Canary Wharf and the City, inequalities worsened. By the time of the pandemic, one in 25 people were homeless — the highest rate in England. Child poverty stood as high as 67 per cent. Unemployment was at 14 per cent, double the average for London. The annual murder rate is the city’s highest. Mayor of London Sadiq Khan has said the failure to build affordable homes in the area despite the billions spent raised a “big question mark” over the legacy of the Olympics.
Surrounding boroughs face similar vulnerabilities — and the constant movement of people between them, as typified by Shah who lives in one, works in another and serves patients from all three — has only amplified challenges during the outbreak of a contagious disease. Despite Newham having the highest numbers in London on the government’s furlough scheme, the second wave landed on a population under huge strain economically as well as from a public health standpoint. Food banks were operating at full capacity, hospitals ran out of oxygen, ambulance shortages were commonplace and local community groups rushed to support families.

“Early on, it was all ‘we’re in this together’ and ‘the virus doesn’t discriminate’. But then it emerged that it did,” says Jason Strelitz, Newham’s director of public health. “Certain populations were not only more likely to become infected and suffer the worst impacts from the virus but also the adverse impacts of trying to control the pandemic and the economic consequences.”
For John Harris, whose family has run the funeral services business T Cribb & Sons in east London for 140 years, these factors resulted in a tragedy of epic proportions. In January, his phones rang constantly. “I’ve been doing this job for the last 49 years and I’ve never experienced anything that has come close to this,” he says. “During the Blitz, the Romford Road [swimming] baths were used as a mortuary. When I just spoke to my dad, he says it sounds worse today.”
Harris, whose staff were working 16-hour days, is frustrated by those who underestimated the severity of the new variant and its impact locally. “I don’t want to take the risk and I don’t want my staff to take the risk,” he says. “But if you are in a war, you can’t say you don’t want to face it . . . This is desperately real. It is a crisis in every sense of the word.”
The soaring case rates and the need to keep working were inextricably linked. Jobs in these areas largely fall into two categories — frontline workers and others in more insecure employment. The situation has long been fragile for those on low-paid zero-hours or shorter-term contracts, for example in hospitality, leisure and retail. Pre-pandemic, up to 36,000 residents in Newham worked below the minimum wage. The worst hit are those in the informal sector, paid cash in hand for shifts.

Community groups say that these people — who may work for restaurants or deliver goods — are now being exploited. “The employer will call in the morning and say ‘come in’ or ‘don’t come in’. They’re being treated like third-class citizens . . . They’re only paid £2 or £3 an hour,” says Elyas Ismail at Newham Community Project, which creates food packages for overseas students who are among the more than 10,000 individuals living in the borough without access to public funds. “Someone even called me once they found out what I’m doing to say, ‘I’ll pay these people £1.50.’ It’s slave labour, people were already taking advantage of them. Covid happened and this has gotten worse.”
In a letter to prime minister Boris Johnson written last May, Fiaz asked that an additional “Covid-19 deprivation premium” be provided to the borough. Areas such as those inside the Covid Triangle have been disproportionately affected after years of local authority cutbacks. By October, the borough was given an extra cash injection but it was still not enough. Speaking to the FT, Fiaz says: “We just don’t have the resources we need.” The pandemic has cost Newham £68m, with the government only providing £38m in funding. “There is a clear shortfall.”
For local businesses, the economic impact has been quick and real. Chiggy Okojie, who works at Mr P Taste of Home, a takeaway restaurant serving African and Caribbean dishes on Upton Park’s Green Street, says it is a hard grind keeping the business going. “Jollof rice, curried goat, oxtail are customer favourites. Jerk chicken, that’s my speciality. I used to make 30 packs and it would go in one hour,” she says.
“Now, some days it’s really very quiet. No one has the money these days. Before we might have 50 customers in one night. Now, only 10.” She tries to keep a brave face but attributes the drop to her regulars just not having the spare cash. “It’s primarily to do with income. Before, people would place a big order so that it would last them through the week. Now only small items.”
Down the road at the Elegance Boutique, which sells elaborate outfits to the Indian, Pakistani and Bangladeshi communities, owner Harmeet Singh says these items are now viewed as unnecessary luxuries. “Pre-Covid, we would get 100 people a day walking in. Now, I’ll be lucky if we can get one or two online orders a week. There are no weddings at all,” he says.
This part of east London has long been a magnet for outsiders. In the early 1900s, it attracted Jewish people from Germany; after the second world war, Indian, Pakistani, Bangladeshi and Caribbean families responded to a government push for a Commonwealth workforce. More recently, newcomers from eastern Europe have moved in. Community connections, cheap housing and easy access to work in wealthier parts of the capital have made Newham the UK’s most ethnically diverse local authority.
Each new influx of people has put its mark on businesses, restaurants and shops. On a single trip down Green Street one can buy an abaya — a long cloak worn by Muslim women; alligator peppers, used to make spicy West African jollof rice; and paan, a south Asian snack of chopped betel nut, a sweet rose-petal preserve and desiccated coconut.
As more and more people sought to call Newham home, housing failed to keep up with the demand. Following heavy bombing during the Blitz, narrow Edwardian terraced houses along winding back streets were replaced by pebble-dashed homes with porches and then state-developed concrete tower blocks that came in the 1960s. Later, uniform rows of houses with front gardens and space for cars were constructed, along with high-rise buildings targeting the commuter class.

Many of these homes are now rundown, with the highest levels of overcrowding in the country. The policies of Margaret Thatcher’s government in the 1980s saw less construction of secure and affordable housing, in the hope that the private sector would take over from local councils. But Newham now has one of the most severe affordable housing shortages in the UK. Some 28,000 people are languishing on the borough’s waiting list and more than 5,500 families with children live in temporary accommodation.
“It has steadily gotten worse over the last decade,” says Stephen Timms, MP for East Ham since 1994. Rogue landlords cram people into unlivable spaces to squeeze cash out of vulnerable individuals trying to save on rent. It is not uncommon for one bedroom in a house to accommodate a family of four or more, with bunk beds set up in living rooms, garages, basements and offshoots of back alleyways, while a dozen or more people will often share a single bathroom.
These problems were exacerbated during the pandemic when Timms says it was nearly impossible for households to distance as required. Even for those lucky enough to be in social housing, Covid-19 only worsened the precariousness of everyday existence.
“Conditions of housing are a moral outrage in the way they were in the 1960s. We are there again,” he says. “I spoke to someone at one of my surgeries recently who lived in a two-bedroom council house — him, his wife and five daughters. In the current situation, it’s almost intolerable. The children all have to do school work indoors, in these spaces — they can’t go out. I don’t know how people cope. That family was absolutely on the edge.” The waiting time for bigger council homes has only got longer. One family, he says, had been waiting for 14 years.
As it has become clear that Covid-19 transmission, morbidity and mortality have been exacerbated by the area’s housing challenges, the council is now providing temporary accommodation to those who live in crowded homes and need to isolate, while sticking to a longer-term plan to build more than 1,000 affordable homes by 2022.
“If you live in a tower block, there could well be tens of people sharing a single corridor and hundreds of people using the same stairwell, lift or entryway. There is so much indirect mixing that inherently happens,” says Shaine Mehta, a GP. “If you catch the virus there are not any spare rooms to isolate. Your idea of physical distancing is just different if this is how you live.”
Devi Solanki could not understand how symptoms manifested so differently among the three generations of her family, despite living under one roof in East Ham. The 47-year-old, who works as a kitchen assistant at a primary school, lost her sense of taste and smell, and one daughter had a short-lived temperature. Her father-in-law, who was recovering from major heart surgery, did not get infected at all — while her mother-in-law did, requiring urgent medical care. But it was her healthy, athletic husband who suffered most of all.
After four hours of treatment in an ambulance outside Homerton University Hospital in late December, he was admitted and sent to intensive care. “That’s when it hit me. I thought, ‘Oh my god. My husband, he is fit, he eats well, he is not overweight, so how is he suffering so seriously?’”

For Ankit Kumar, an intensive care doctor who has worked at a series of east London hospitals over the past year, it was obvious early on that those requiring ventilators and other organ support were predominantly from black and ethnic minority populations. “Initially we thought it was just the area. But when the data started to be published, we saw that it was a higher proportion of Bame people versus the demographic of the area,” he says. “By the time they get to intensive care, death is the expectation and survival is the exception.”
Speaking during January’s peak, Kumar said the outsized impact of the virus on ethnically diverse boroughs meant the pressure on local hospitals was unparalleled. Around 72 per cent of Newham’s population are from Bame backgrounds, compared with 44 per cent in London broadly. Redbridge stands at about two-thirds.
It was so bad there was a backlog in the mortuaries. “We have had to keep the dead where they are. Dead for hours, with the curtains drawn, while they wait for mortuary space. For some patients who are awake, it’s quite hard for them to see that. They know that the person in the bay next to them is dead.”
In June last year, a Public Health England report found that people from black, Asian and other ethnic groups were more likely to die from Covid-19 than white people. “People of Bangladeshi ethnicity had around twice the risk of death when compared to people of White British ethnicity. People of Chinese, Indian, Pakistani, Other Asian, Caribbean and Other Black ethnicity had between 10 and 50 per cent higher risk of death when compared to White British,” the report says.

Minority groups tend to fall into those most exposed to infection — because of how and where they live and work — and those with increased susceptibility to the worst outcomes because of comorbidities, but why some people suffer more is unclear. “A high proportion of ethnic minority people live in deprived areas. But you can’t tease out which one is the key driver of not only getting the coronavirus but also feeling the worst effects of it,” says Nishi Chaturvedi, a professor of clinical epidemiology at University College London.
In poorer neighbourhoods people tend to have worse diets and less opportunity and green space for exercise, which over time increases their chances of chronic diseases. Now the pandemic is forcing a conversation about structural disparities and about the role decades of racial discrimination has played. “Social inequalities have got wider since the 1970s and this has impacted health,” she says. “You can get the Tube from Newham to South Kensington. But there is a much higher health expectancy in South Kensington.”
However, doctors such as Kumar say the virus has been more indiscriminate, hitting rich families too. “People tend to think it’s poorer people alone that are more likely to get Covid. But we had some very wealthy Asian people come through intensive care who died from Covid too. No one can explain this.”
Public Health England noted that the historical experiences of black and other minority groups might mean they are less likely to seek help when it is necessary, ultimately having an impact on longer-term health. A group of UK academics recently argued that access to medical care is also determined by a person’s ability to use services “with ease, and having confidence that you will be treated with respect”. This can be “hindered by language barriers, patients’ attitudes towards healthcare providers and the behaviour and attitudes of healthcare professionals towards minority patients”. The effects of racial discrimination in wider society also play a part in why some minority groups are hesitant to take up a Covid-19 vaccine.

There is also a link between diseases such as diabetes and the increased susceptibility to the virus. “Not only are conditions such as diabetes present among lower economic social groups, but certain ethnicities are also more likely to have them,” says Naveed Sattar, a professor of metabolic medicine at the University of Glasgow. “Diabetes is definitely over-represented in the people who died.”
Scientists are investigating genetic determinants that might enhance susceptibility to infection but it is complex. Genetic differences in people of the same ethnicity are more common than those between different minority populations, meaning conclusions about whole groups will likely be wrong. While ethnic minority groups suffer from chronic diseases differently, before the pandemic they had higher life expectancy at birth than the white population. However, “the impact of Covid-19 has been so significant that it has reversed the previous picture and many ethnic minority groups now have higher overall mortality”, say the authors of a new King’s Fund report.
This has become sadly obvious to many of those who live and work in this part of east London. Imran Ali is a 34-year-old anaesthetist at the Royal London Hospital, who lives in Redbridge. He has been part of teams caring for those who could not breathe and whose bodies were rapidly shutting down. Many were from the Covid Triangle.

“I can remember the people that I put to sleep and that didn’t come back,” he says. “I’m the last face people see.” Ali would stand over them as they closed their eyes and then help put them on ventilators, with tubes and machines taking over basic functions. He watched as families said their goodbyes. He did not expect to be doing the same thing with one of his own family.
Last November, Ali’s 68-year-old father-in-law Abdul-Razaq Abdullah, a GP in the east London suburb of Rainham, was isolating alone at home after experiencing Covid-19 symptoms. The family believes he caught the virus from a patient. When Abdullah stopped responding to texts and did not answer the doorbell, the fire services forced entry into his house only to find him collapsed on the sofa. His lips were blue, his oxygen levels were “barely detectable” says Ali, and he had to be rushed to hospital.
Doctors asked Ali and his wife to tell Abdullah that he would have to be put on a ventilator. “Because of my job, I knew something bad was going to happen,” Ali says. “I wanted to be honest with him. One of the last things I said to him was: ‘This could be the last time I see you.’” After a month in a coma, Abdullah died.
For those in the Covid Triangle, it is not uncommon to know of dozens of individuals who have been struck by the virus. Newham expects its death rate over the past two months to exceed that of early 2020. Zoom funerals and prayer meetings for the dead have been weekly events. The area has become emblematic of other poorer regions in the country with large minority populations. How it recovers after the pandemic may signal whether other deprived areas will be able to turn around their fortunes. “We haven’t seen the full impact of this yet,” says public health director Strelitz. “Where we go from here no one can be sure.”
Mia Gray, an expert in local authority funding at the University of Cambridge, says Newham’s past will hinder its recovery. “Council budgets across the country have taken an enormous hit over a decade of austerity, affecting their ability to function, their ability to have expertise on different issues and, importantly, the provision of a local safety net,” she says. “These different strands got interwoven into the bigger problems around the pandemic. That has a very long-lasting legacy and it is not something that lifts when government restrictions end.”
Sadiq Khan recently accused the government of “imposing a new era of austerity on public services”. He says that inadequate local funding means he is rebuilding the city “with one arm tied behind my back”. By January, the Greater London Authority had spent £84.7m — not covered by the government’s funding initiatives — to support London through the pandemic, a figure that is likely to have increased during the current lockdown.

In Newham, educational outcomes had improved in recent years. But homeschooling in cramped conditions and digital poverty, with multiple siblings sharing a single device, has put progress into reverse and young people most at risk. Kevin Jenkins, who runs Ambition Aspire Achieve, a charity supporting Newham’s youth, says: “As we come out of this current lockdown, how do you support these kids? Remember, the basic services weren’t there in the first place, from play schemes to youth projects.”
One beacon of hope, says Lee Taylor, a priest at St Michael & All Angels church in Manor Park, is that the pandemic has “galvanised” local networks. The church has worked with mutual aid groups on everything from promoting the benefits of vaccines to arranging deliveries of medicines to those shielding, together stepping in to provide a buffer in Newham. “Where perhaps we haven’t worked together in the past, we will have to in the future,” he says, “particularly if this happened again.”
For Mayor Fiaz, this is key to building back. Even as the borough pushes to secure adequate funding, Newham has sought to prioritise the health, wellbeing and happiness of residents as its prime measures of Covid-19 recovery and economic success.
Such intangible metrics are difficult to track but the borough realises quick progress in more rudimentary areas is key to achieving these goals, including plans to build new homes, upgrade existing council houses, create new youth facilities, set new standards for local working conditions and provide better mental and physical health support through community outreach. Speed is crucial. It is only a matter of time, Fiaz says, before “there will be another deadly virus that will challenge the community again”.
Preparing for the post-pandemic future will also require grappling with the past. Gray says that Newham’s experience with coronavirus has brought into focus what has been hidden in many parts of the UK for years and the dire consequences of inadequate government support. Should the prime minister take seriously his ambition to “level up” and revive the fortunes of those areas left behind, recent events should force a rethink of the role of the state.
“There are often these moments of restructuring that come after such crises,” says Gray. “But in the past, we have been able to look away, and my fear is that we will continue to look away. What is visible now will become invisible again.”
Anjli Raval is the FT’s senior energy correspondent
Follow @FTMag on Twitter to find out about our latest stories first. Listen to our podcast, Culture Call, where FT editors and special guests discuss life and art in the time of coronavirus. Subscribe on Apple, Spotify, or wherever you listen.
Comments